Future Horizons:
10-yearhorizon
Risk maps developed
25-yearhorizon
Rabies eliminated
Pathogens can come from wild species — as with SARS-CoV-2, which originated in bats — or from domestic animals, as with MERS, which came from camels. Intensified farming systems create significant risk, as evidenced by the recent avian influenza outbreak.12 While researchers have devised global risk maps showing regions of the world where the risk is highest, in practice the high-risk areas are too large to be practicably managed, so it is vital that we create more finely grained maps.
Understanding the risk also requires a better understanding of the necessary conditions for inter-species pathogen transmission. For example, it is often hypothesised that the risk is greatest when humans push into a new area and thus come into first contact with species whose pathogens might evolve to use humans as hosts. However, often when humans move into a new area they degrade wildlife habitat, driving out or exterminating many animal species. This might reasonably be expected to reduce the risk of a disease crossing over. Understanding human-animal ecosystem interactions is thus likely to be key.
A vital part of this will involve data-sharing and integrated practice in human and animal health research and treatment. At the moment, human and animal researchers tend to work in parallel, with little contact across the divide. Given the threat of zoonotic disease, this situation is not conducive to the prevention of future outbreaks. More use also needs to be made of social and anthropological science, and local knowledge and insight, especially when resulting from “citizen science” projects, although progress is being made in these areas.13
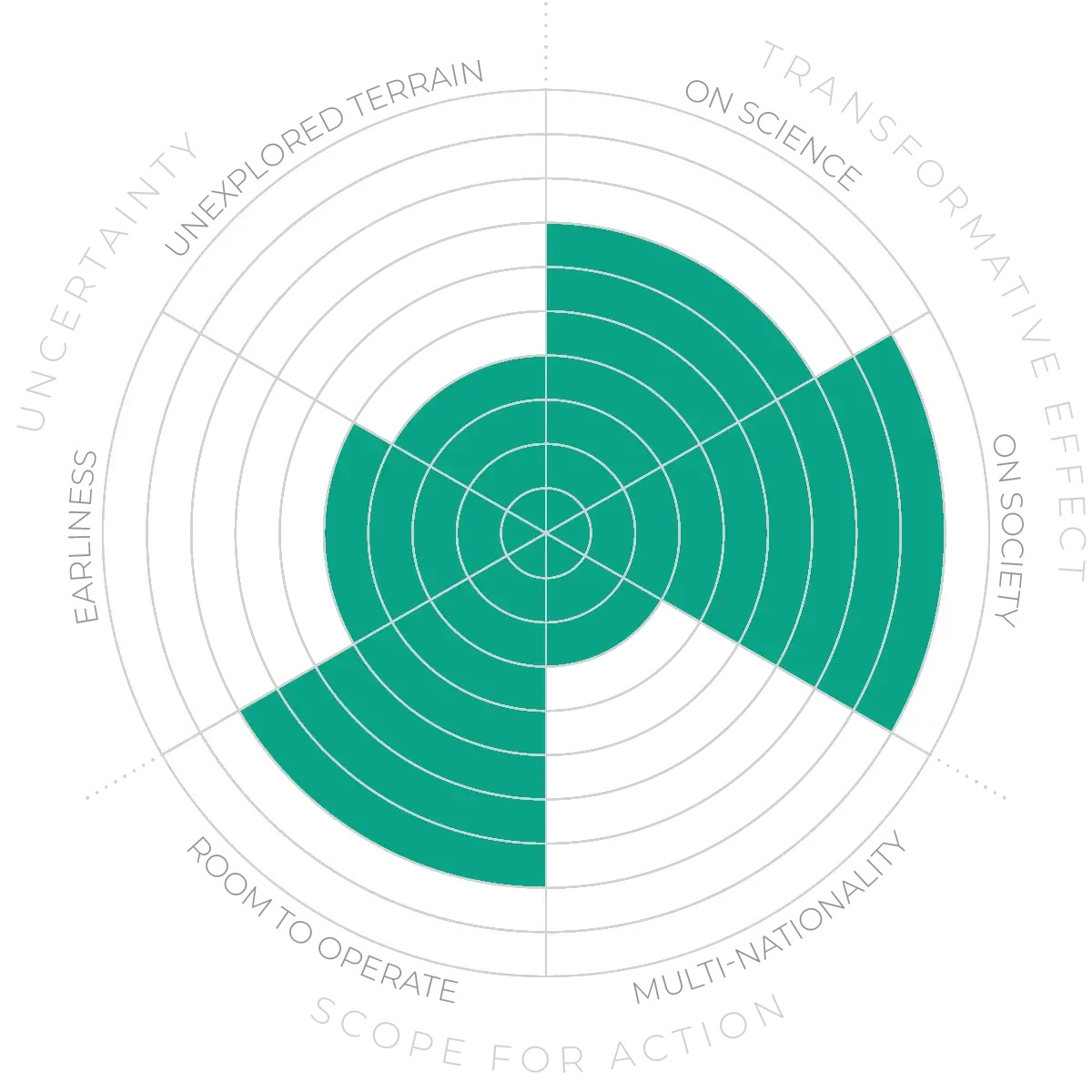
Zoonotic disease - Anticipation Scores
The Anticipation Potential of a research field is determined by the capacity for impactful action in the present, considering possible future transformative breakthroughs in a field over a 25-year outlook. A field with a high Anticipation Potential, therefore, combines the potential range of future transformative possibilities engendered by a research area with a wide field of opportunities for action in the present. We asked researchers in the field to anticipate:
- The uncertainty related to future science breakthroughs in the field
- The transformative effect anticipated breakthroughs may have on research and society
- The scope for action in the present in relation to anticipated breakthroughs.
This chart represents a summary of their responses to each of these elements, which when combined, provide the Anticipation Potential for the topic. See methodology for more information.