Future Horizons:
10-yearhorizon
Public health systems strengthened
25-yearhorizon
Early-warning system established
A key research challenge is to understand how outbreaks arise and ultimately to predict them. It is therefore crucial to study each disease in the multiple species it infects and to track it as it moves from one to another. Alongside that, we must gather genomic data so that outbreaks can be traced back to their sources – which can then be monitored.
This information can then be harnessed to predict outbreaks, and to rapidly detect them when they occur. Better surveillance and early-warning systems are essential. It will be important to develop cheap, effective and easy-to-use rapid testing tools, ideally able to detect several pathogens with one test. This will be particularly relevant in communities where human and animal populations are in regular close contact.
Our preventative strategies will be most effective if we approach human health in more social-ecological terms. For instance, changing animal husbandry practices will slow down the reshuffling of pathogen genetics and reduce the chances of generating new zoonotic diseases. One framework for this type of approach is One Health, which aims for cross-disciplinary work integrating human health, animal health and environmental health.21 There is also a framework called Planetary Health, formally launched by the Rockefeller Foundation and The Lancet in 2015.22 This draws on the concept of “planetary boundaries” that should confine human activity. The exact definitions of these concepts are not fully agreed, and it is not clear which provides the better framework. Bibliometric analyses suggest that researchers focusing on one or the other tend to emphasise different topics. However, there is also a clear complementarity, and the overarching concept is widely agreed to be a desirable framing for the future of public health.
Alongside this, there is an urgent need to redevelop and modernise public health systems in the face of the threat from infectious disease.23 In many developed countries there has been considerable focus on developing pharmaceutical and hospital treatments. But while these are obviously essential, they are only part of the picture. For example, many countries have poor capabilities for testing and contact tracing, and their welfare systems do not provide adequate support for containment measures such as self-isolation.24 In addition, a combination of better ventilation and air-filtration systems can reduce the spread of airborne viruses like SARS-CoV-225 – and reduce the enormous harm from air pollution into the bargain.26
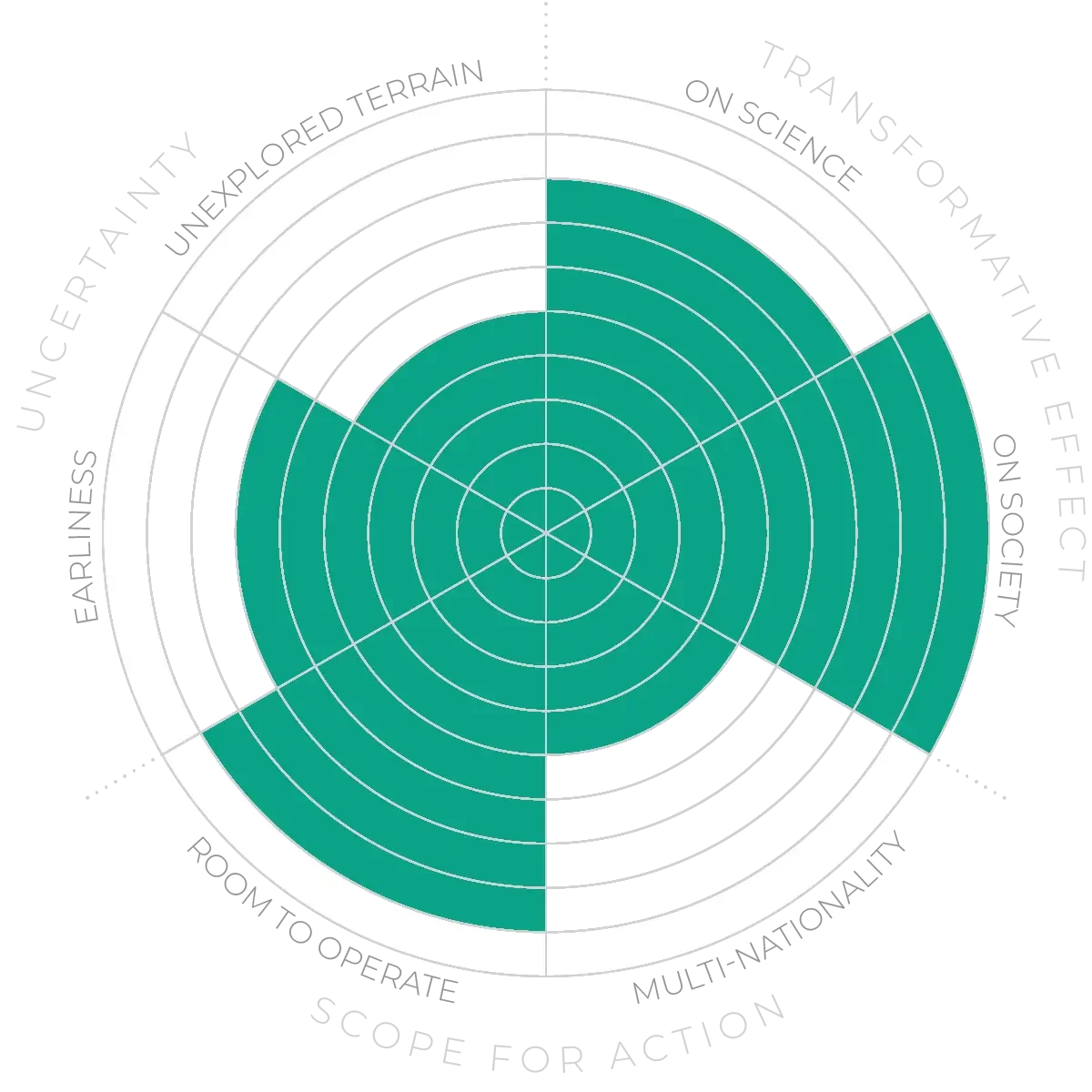
Outbreak prevention - Anticipation Scores
The Anticipation Potential of a research field is determined by the capacity for impactful action in the present, considering possible future transformative breakthroughs in a field over a 25-year outlook. A field with a high Anticipation Potential, therefore, combines the potential range of future transformative possibilities engendered by a research area with a wide field of opportunities for action in the present. We asked researchers in the field to anticipate:
- The uncertainty related to future science breakthroughs in the field
- The transformative effect anticipated breakthroughs may have on research and society
- The scope for action in the present in relation to anticipated breakthroughs.
This chart represents a summary of their responses to each of these elements, which when combined, provide the Anticipation Potential for the topic. See methodology for more information.